
Contact
Department
Pharmacology
Jason O’Connor, Ph.D.
Associate Professor of Pharmacology
Personal Statement:
View a video introduction to Dr. O’Connor’s lab
The immune system and the brain engage in an exquisite bidirectional communication network to orchestrate the host response to infection. This adaptive response includes physiological, metabolic and behavioral changes. The innate immune system is not only activated by pathogenic bacteria and viruses, but it often becomes chronically activated as a result of disease or even the normal aging process. When neuroimmune processes become dysregulated, there is a substantial increase in the risk of developing depressive disorders for individuals affected by these chronic inflammatory conditions. The neurobiological mechanisms and immune substrates underlying these immune-brain interactions are poorly understood.
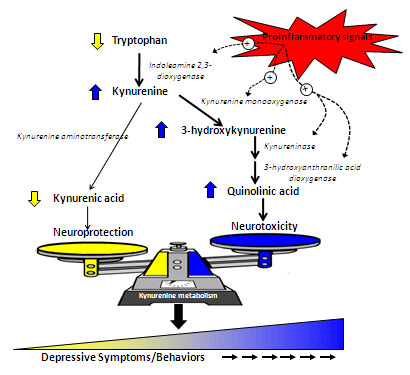
My research is focused on understanding the biological basis of inflammation-related depressive disorders. To that end, we have developed clinically relevant mouse models of inflammation-induced depressive behavior. Using these models, we have identified a critical role for altered tryptophan metabolism in mediating depressive-like behavioral changes induced by peripheral immune activation. The essential amino acid, tryptophan is the biologic substrate for the formation of serotonin. However, during inflammatory conditions, an alternate tryptophan degrading pathway, called the kynurenine pathway, is activated. In macrophages and microglia, increased flux of tryptophan through this pathway produces a number of neuroactive kynurenine metabolites with the capacity to increase oxidative damage within the brain and to interact, both directly and indirectly, with the other neurotransmitter systems.
We are working to elucidate
- How this metabolic network is regulated between the brain and periphery
- Which kynurenine metabolites actually effect behavioral changes
- How they impinge upon the function of neural circuits relevant to behavior and ultimately
- How these molecular pathways contribute to a deterioration in the quality of life of various populations affected by chronic inflammatory diseases.
Our goal is to provide new information and understanding of complex neuroimmune interactions that can be taken to the clinic and used to develop more effective therapeutic strategies to prevent or treat comorbid depression.
Research
| • neuroimmunity |
• neuroinflammation |
| • anxiety |
• depression |
| • behavior |
• kynurenine |
| • cytokines |
• glia |
Awards & Accomplishments
- Briscoe Women’s Health Scholar – 2016
- Morrison Trust Award
- Hogg Foundation for Mental Health Grant
Affiliations
- Norman Hackerman Advanced Research Program (003659-0010-2012) | 2014-2016
Neurotoxic tryptophan metabolism by microglia: novel insights into the neuropathology of suicide
OBJECTIVE: to explore the role of microglial activation and subsequent metabolic changes within the prefrontal cortex on suicide using both postmortem human brain tissue and a rodent model of inflammation-induced cognitive inflexibility.
- NIH/NIMH, R01 (MH090127)- 2.4 CY | 2010-2015
Biobehavioral Role of Brain Kynurenine Metabolism in Mental Illness
OBJECTIVE: to investigate the role of the placenta and sexual dimorphism in transducing maternal immune signals to the fetus that drive the development of autism-like behavior.
- IIMS/SOM (Co-PI) | 2014-2015
Maternal immune activation, the placenta and development of autism spectrum disorder
OBJECTIVE: to investigate the role of the placenta and sexual dimorphism in transducing maternal immune signals to the fetus that drive the development of autism-like behavior
- Morrison Trust (NCE) | 2013-2015
Neurodvelopmental consequences of dysregulated prenatal tryptophan metabolism: implications for autism spectrum disorder
OBJECTIVE: to determine whether maternal or fetal kynurenine metabolism contributes to neurodevelopmental consequences of prenatal maternal immune challenge with poly I:C
Lab Members

Mustafa Mithaiwala
Neuroscience Graduate Student |
|
|
|
|
Publications



